Recently, a philanthropic couple I know invited me to accompany them to Nepal on a fact-finding mission for The World of Children Awards. One of the first things we discussed was how they should manage their medications while traveling, particularly through several different time zones.
This question often arises, and there is no one right answer. Some medications call for maintaining a consistent level of the drug in your system at all times, which often means taking it at a specific and consistent time of day. People taking antidepressants such as Prozac®, Cymbalta®, and Paxil® and neuropathic drugs such as Neurontin® and Lyrica®, for example, must be extra vigilant as they are at greater risk for mild to severe withdrawal symptoms if they miss a dose. Exactly how your dosage instructions will change while traveling depends on the medications that you take and your doctor’s recommendations.
According to the American Diabetes Association, patients who take insulin typically do not have to adjust their doses if they cross fewer than five time zones. But it’s even more nuanced than this: traveling east will shorten one’s day and may necessitate a reduction in insulin (particularly for shorter flights) because insulin doses then would be given closer together than normal and could raise the risk of hypoglycemia. Alternately, traveling west means a longer day, so insulin doses may need to be increased. Talk to your doctor, as differing times of departure and prolonged flights might require a more adaptable approach. This could apply to other medications as well.
If you are someone who takes medications regularly, it’s crucial to talk with your doctor or doctors before you leave. You can’t rely on Internet chat boards to tell you what to do as every medication and every person is different. I recommend scheduling an appointment at least four weeks before you travel, as your doctor might suggest changing the times you take your medications before you go to match the time zone you’ll soon be in.
Always get prescriptions refilled before you travel overseas. A good rule of thumb is to bring at least twice the medication you need for the length of time you’ll be away. Getting a refill may not be difficult if you’re traveling in the US, but even if you are, it can’t hurt to bring extra, just in case.
Since you will be travelling aboard your own aircraft, the possibility of lost luggage is minimal, but it’s always a good idea to carry a one- or two-day supply of any critical medications on your person.
Check regulations before you fly. According to the Mission of the Bureau of Consular Affairs, medications should always be transported in their original, labeled bottles, along with documentation of the prescription. Although you’re not likely to be subject to TSA rules, it’s a good idea to check the laws of the destination country for any restrictions on importing your medications. Some countries require special permission or licenses in advance. Some, such as Japan and Australia, and parts of the UAR, like Dubai, don’t allow the import of specific medications under any circumstances, and others, such as the UK, allow only a predetermined amount of certain medications common here in the US (including some anti-anxiety drugs and pain relievers). Contact the consulate/embassy of your destination country before you go.
Now that we’ve got all that covered, enjoy your trip and travel safe. BAA
 Is There An App for That?
Is There An App for That?
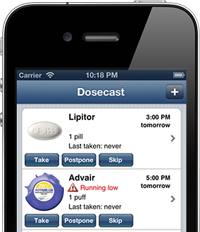
If you have a smartphone or an iPad, look into the Dosecast app, declared “best of breed” by The New York Times. Using Dosecast, you set daily, weekly, or monthly medication notifications, with or without WiFi. You can postpone reminders if you want to skip a dosage. This app even adjusts your schedule to different time zones. However, don’t rely solely on any app, as even the best tool is fallible, can break, or can be lost or stolen.
Christopher Sidford, MD, founder of Black Bag Global Emergency Medicine, is a former U.S. Navy officer who has taught and practiced emergency medicine for 25 years, from Boston and San Diego to the Arctic Circle.


 Is There An App for That?
Is There An App for That?

